Interview with Dr Christopher Hess of UCSF and Kheiron Medical: Where the Rubber Meets the Road – UCSF and Kheiron partner in pioneering Center for Intelligent Imaging
Article by Dr Christopher Austin, Chief Medical Officer, Kheiron Medical
Deep learning has become democratized over the past two years. Anyone with access to data, open source software and a Graphics Processing Unit (GPU) can tinker and build something that works.
However, this approach falls short in healthcare, where consistent quality and patient safety are at stake. It is one thing to create an algorithm, but an entirely different endeavor to validate, package and safely deliver in clinical practice.
A handful of companies have pushed through regulatory barriers (CE marking in Europe and FDA approval in the USA) and in some cases have established functional integration with hospital systems. However, none have yet proved that real-world outcomes can be positively impacted by this technology through robust prospective clinical trials. Even more importantly, none have demonstrated that their algorithms can safely and accurately generalize across healthcare systems and geographies – an essential ingredient for broad clinical acceptance.
Putting medical Artificial Intelligence (AI) software through its clinical paces is the focus of UCSF’s newly announced Center for Intelligent Imaging (ci2). Kheiron could not be more proud to be chosen, along with NVIDIA, as the first launch collaborators for this important UCSF initiative. Clinical rigor has always been at the heart of what we do. Following this core value, the initial focus of our work, together with UCSF, represents an alliance with the world-renowned UCSF Breast Imaging team to demonstrate that our deep learning software, Mia™, can be safely deployed and demonstrate meaningful impact on UCSF’s ethnically diverse breast screening population.
I had the privilege of interviewing the visionary behind the Center for Intelligent Imaging, Dr. Christopher Hess, MD, PhD, Professor and Chair of the UCSF Department of Radiology and Biomedical Imaging. Dr Hess views AI as a transformational tool for the field of radiology.
Why have you launched the Center for Intelligent Imaging (ci2)?
In our current climate, medical AI is inflated by hype. The promise of AI is becoming overshadowed by its failures, and we risk missing the opportunity to use it to make the quality and safety of imaging better and to bring more to our patients. There are few environments where algorithms are systematically being put through their paces. I’m keen to make UCSF a place where new AI technology is not only developed, but also where it is evaluated for its merit and used in everyday practice. We’re intent on not only inserting AI into our clinical workflows, but also showing its inherent value to patient care. Using cancer diagnosis as one example, I would ask the following question– can we detect malignancy earlier, initiate life-saving treatments at earlier points and reduce overall morbidity and mortality?
Personally, I’m also excited about the potential for some AI tools to bring operational efficiency to our practice. Because imaging plays such a large role in medical decision-making, the volume of studies that we are faced with is increasing at an unprecedented rate. As a radiologist, the work is getting harder and harder and burnout is endemic. We simply can’t keep up. The center will prioritize AI solutions to enable radiologists to practice at their license by improving workflow, integrating data from multiple sources, and reducing inefficiency.
Why UCSF?
We have a long and storied history of driving innovation in the field of Radiology. MRI is a great example. It started as a research tool, but our group had a vision that it would become a clinical tool. In the early days of MRI, patients were driven to our research facility at Oyster Point, where our first MRI scanner was situated, so radiologists could show just what this new technology could bring to diagnosis. So many stories of innovation from that time.
I am convinced that the next generation of imaging technology will involve more advanced analytics and integration of data from multiple sources. How can we accelerate that as an academic enterprise? My view is that we do this by partnering with the right people and putting the technology in front of radiologists, so that we can kick the tires on it.
Why are there so few impactful AI solutions today?
I would say there are two primary reasons. First, I am not convinced we are answering the right questions using this powerful new technology. Neither industry nor physicians in practice are entirely sure what problems they’re trying to solve with AI. So far there have been a number of algorithms developed, but most address narrow questions and are simply not that useful. Second, medical imaging is hard! Interpreting images involves not only pattern detection, but also context, knowledge about anatomy and disease, and above all, human judgement.
Ultimately what we need to do is develop AI solutions that set the bar higher. For example, I think triaging cases into normal and not normal is a good start. If it’s possible to set aside a case that’s normal with high enough accuracy, such that a human doesn’t need to lay eyes on it, it would be possible for us to focus on more challenging and complex cases where our expertise is so important.
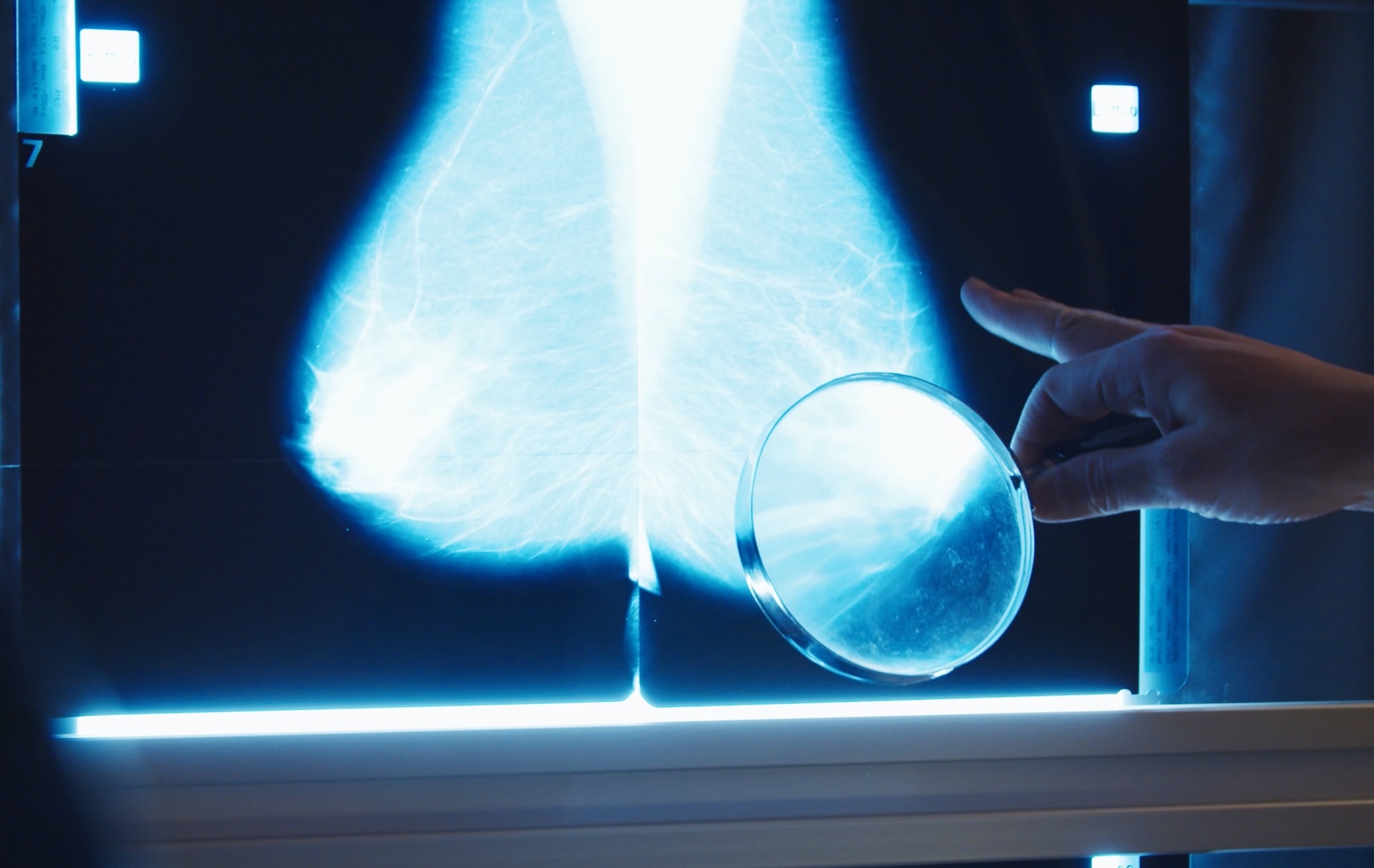
Why is mammography the first use case for UCSF?
Globally, there is an epidemic of breast cancer. It affects every woman’s life, either because they’ve had it or know someone who has. We need to make a dent in this horrible disease.
We all know the story of Computer Aided Diagnosis (CAD) software and why that didn’t work. It was a performance issue, but it was also a workflow issue. If you show a radiologist a bunch of erroneous marks on a mammogram, and it takes them more time, not less, to read the mammogram, with no improved accuracy, no one will want to use it. But if AI can more accurately reassure the screening radiologist, accelerate their interpretation, and reduce the anxiety of the patient, that’s transformational.
Working with Kheiron Medical, we aim to move beyond traditional screening models and leverage AI to develop a more personalized screening program in the future.
What will the world of radiology look like 10 years from now?
I think our role as ‘pattern detectors’ will diminish. I expect that radiologists will play an even greater role than they currently do as ‘care traffic controllers’ and ‘curators of information,’ with imaging data serving as just one piece of each patient’s journey. I also think we will see much more consistency of diagnosis as a result of AI, and fewer misses.
Finally, I’d like to see a system in which radiologists really enjoy their work, to break the trend where imaging volume increases at a rate that is so much higher than the number of radiologists and radiology hours. Radiologists need to be able to practice at the top of their license.
What’s next for the ci2 ?
ci2 will operate very much like a startup company within UCSF, so it will have a lot of autonomy and nimbleness to make decisions and to move quickly. Our inaugural partners are NVIDIA and Kheiron Medical. We are set on working closely with exactly the right people who share the same commitment and vision to bring AI into clinical practice and join in this journey together.
If you are attending RSNA 2019 and would like to hear more about the partnership, make sure you attend our lunch and learn session to hear directly from our UCSF partners including Dr. Christopher Hess.
When: Tuesday 3 December, 12.30-1.30pm
Where: McCormick Place, South Building, Level 4, Room S403A
To guarantee your place at the lunch & learn we highly recommend booking in advance which you can do here.
For more information about the lunch and learn as well as other opportunities to hear from Kheiron at RSNA please head over to our dedicated RSNA webpage.
UCSF
